Contrast Transport
Whole Organ Perfusion / Contrast Transport / Cathlab Diagnostics / Permeability Estimation
Perfusion Imaging
Clinically, localised reduction of blood flow can be visualised using non-invasive imaging modalities such as magnetic resonance imaging or computed tomography. Both work on the principle of following the passage of an injected contrast agent, which acts as a surrogate marker for the blood. However, due to the in vivo properties of contrast agent, both imaging-wise and transport-wise, the interpretation of the resulting images and quantification of absolute perfusion levels may be confounded.
Three slices of 2D perfusion MRI With a perfusion defect marked by the yellow arrows. Courtesy of Prof. Eike Nagel, King’s College London.
Contrast Agent Transport Modelling and Virtual Imaging
Transport processes through the vascular network and myocardium can be modelled using the advection-diffusion-reaction equation, in conjunction with a porous or a poroelastic medium model of the underlying perfusion. Furthermore, the solutions of this system can be paired with in silico imaging, whereby MR or CT images are generated via simulation. We have developed novel finite element implementations of multi-compartment poroelastic transport, using in the in-house modelling software, CHeart. These developments allow us to simulate the complete loop from imaging to modelling, and back to imaging again, facilitating validation as well as novel investigations as outlined below.
SImulated contrast-enhanced myocardial perfusion imaging
Effect of Temporal Sampling
The pulsatile flow and the flow-contraction interaction was studied using the poroelastic perfusion & transport models. The results showed that common clinical indices for perfusion (such as peak upslope) are highly sensitive to the particular point in the cardiac cycle at which the image is taken. Such differences are difficult to characterise by imaging alone, due to the limited temporal resolution and extent. In addition the degree of sensitivity itself was found to depend on the trasnsport properties of the contrast agent.
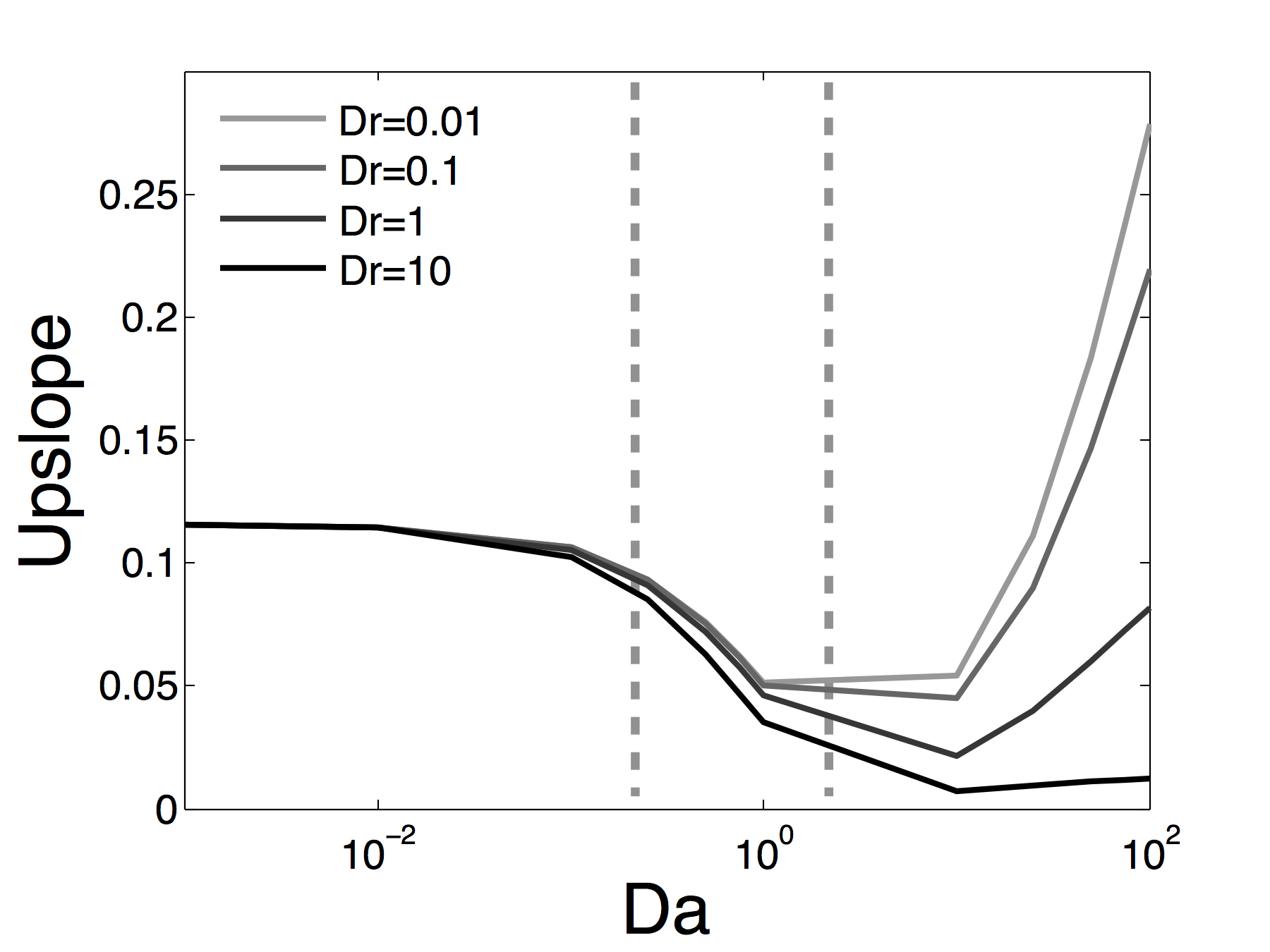
Sensitivity analysis of perfusion image signals to contrast agent parameters. (Originally published in Cookson et al. (2014). Reproduced here under the Creative Commons License 3.0 (http://creativecommons.org/licenses/by/3.0/). )
Matching Contrast Agent to Imaging Protocol
The effect of varying properties of the contrast agent on perfusion images and derived clinical indices were investigated in greater detail. The model results showed that when the perfusion reserve index was evaluated using a moderately freely-diffusive contrast agent, the most sensitive results can be achieved as opposed to using blood-bound agents. Conversely, if perfusion quantification via signal deconvolution is used, then a contrast agent with limited diffusive behaviour may be preferable. Further details of this study can be found in Cookson et al. (2014).